Podcasts your mind will love
Introducing an eclectic mix of podcasts from Headspace Studios. Get some perspective, learn something new, and hear advice from our expert teachers.
It’s all available in the Headspace app. Start now and get a special 30-day free trial.
On mobile and have the app installed?
Listen here
Explore our shows

New: Dear Headspace
Our mindfulness teachers answer questions from our community — about life, work, or anything else that keeps you up at night.
Listen now
Submit your question

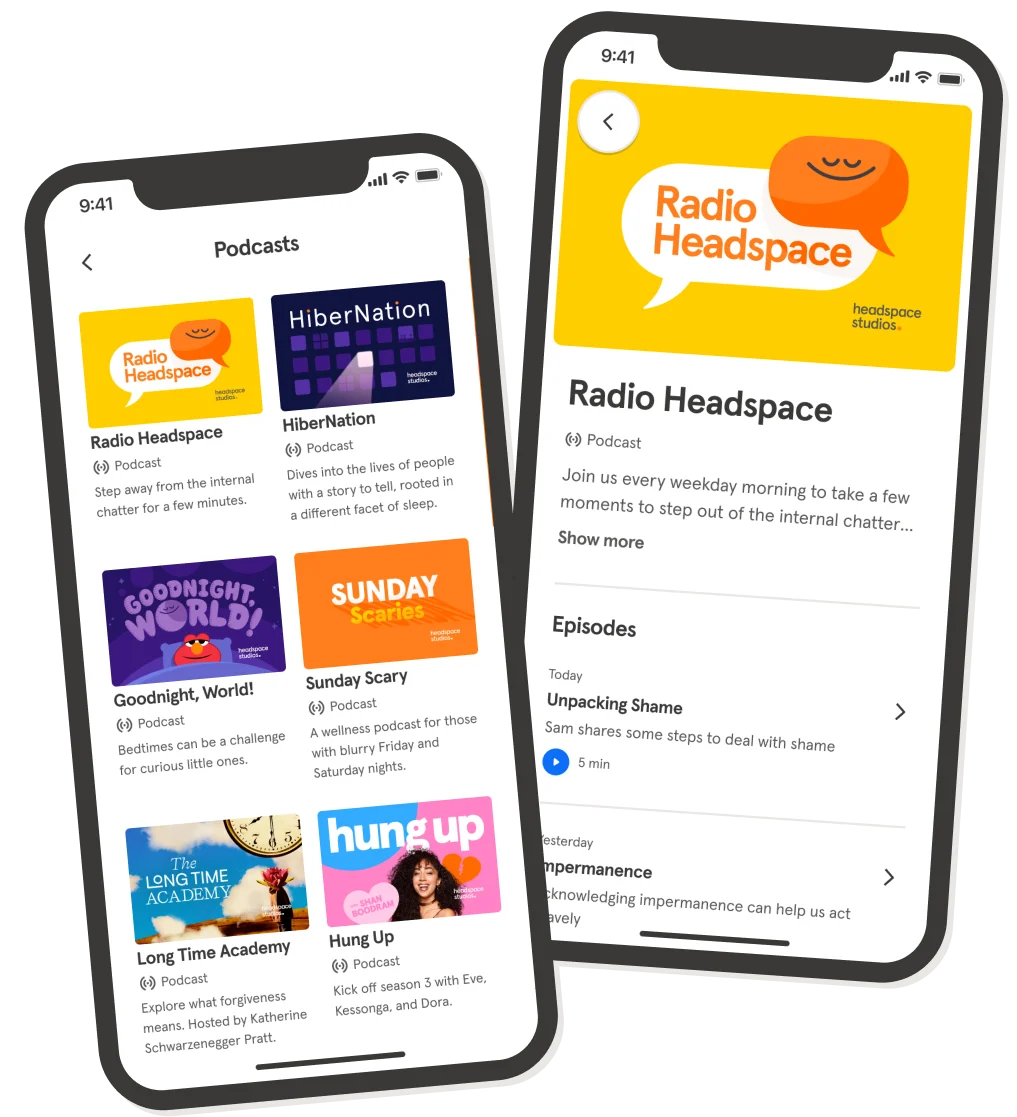
Radio Headspace
Step away from busy thoughts with Headspace mindfulness teachers every weekday.
Listen now

Sunday Scaries
Reframe how you feel about Sundays, and the week ahead, with our teacher Dora Kamau.
Listen now

Goodnight, World!
Kids can join their favorite Sesame Street characters to calm their minds for better sleep.
Listen now

The Yes Theory Podcast
Find happiness out of your comfort zone with Yes Theory founders Ammar, Matt, and Thomas.
Listen now

The Long Time Academy
Changing how we engage with time can improve our lives now, and solve problems of the future.
Listen now

HiberNation
Host Mallika Rao takes listeners on a personal investigation into a nation not sleeping.
Listen now

Hung Up
Relationship expert Shan Boodram helps guests still stuck on their exes finally move on.
Listen now
Listen now in the app
Need a mindful moment on the go? Critically-acclaimed shows from Headspace Studios are available to stream on all platforms, and Headspace members can listen in-app.
On mobile and have the app installed?
Listen hereDiscover what mindfulness can do for you

Get more restful sleep
Find your perfect bedtime routine with hours of relaxing music, sounds, bedtime stories, and exercises.

Get more goodnights
Access our entire library of meditations, sleep sounds, yoga and fitness, and focus music.

Prioritize your mental health
Discover guided meditations and programs that help you stress less and learn to handle new challenges with ease.
- © 2024 Headspace Inc.
- Terms & conditions
- Privacy policy
- Consumer Health Data
- Your privacy choices
- CA Privacy Notice